Key Performance Metrics for Mechanical Ventilators:
Achieving Optimal Patient-Ventilator Interaction
Mechanical ventilation is a cornerstone of critical care, providing vital respiratory support to patients unable to breathe adequately. Achieving optimal patient-ventilator interaction is essential for improving patient comfort, reducing work of breathing (WoB), and preventing complications such as ventilator-induced lung injury (VILI).2 To achieve these outcomes, it is essential to understand key performance metrics, address challenges arising from patient-specific factors, and implement advanced ventilatory strategies.1
Effective triggering and cycling ensure the ventilator synchronizes with the patient’s spontaneous breathing. Below are key types of asynchronies: 14
1. Trigger Asynchrony
Ineffective Triggering: The patient attempts to initiate a breath, but the ventilator fails to recognize the effort, often caused by a high auto-PEEP preventing sufficient pressure gradient.3 or a weak respiratory effort due to muscle fatigue or sedation. 6
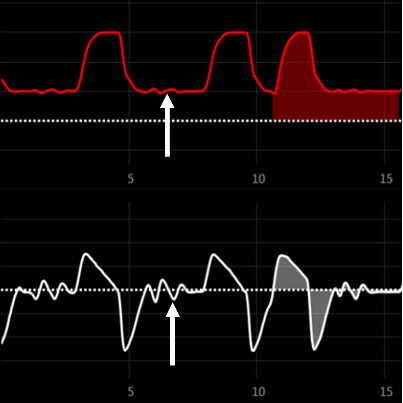 Figure 1 Missed Trigger: Wasted patient breath attempts due to inappropriate trigger settings
Figure 1 Missed Trigger: Wasted patient breath attempts due to inappropriate trigger settingsAuto-Triggering: The ventilator delivers a breath without patient effort, often caused by circuit leaks, cardiogenic oscillations, or excessive sensitivity settings. 5
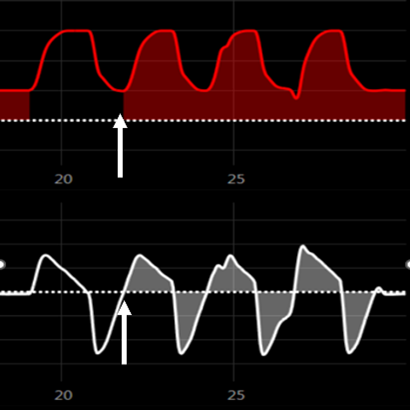 Figure 2 Auto Trigger: Initiation of a breath, without any patient interference.
Figure 2 Auto Trigger: Initiation of a breath, without any patient interference.
2. Flow Asynchrony
- Insufficient Flow: The ventilator fails to meet the patient’s inspiratory demand, leading to air hunger and increased work of breathing. 9
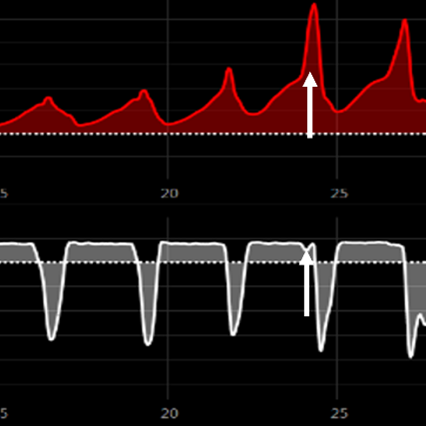 Figure 3 Flow Starvation: The flow setting does not meet the patient's inspiratory demand.
Figure 3 Flow Starvation: The flow setting does not meet the patient's inspiratory demand.
Excessive Flow: The ventilator provides a flow rate higher than the patient’s need, resulting in increased airway pressure and potential discomfort.
3. Cycle Asynchrony
Premature Cycling: The ventilator terminates inspiration before the patient has completed their breath, leading to increased inspiratory effort and patient discomfort.
- Delayed Cycling: The ventilator prolongs inspiration beyond the patient’s natural effort, causing breath stacking and increasing work of breathing.
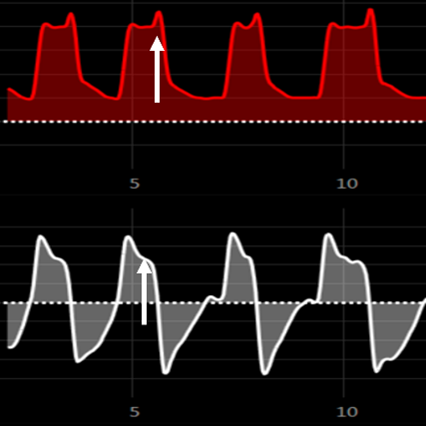 Figure 4 Delayed cycling: Patient inspiratory time is shorter than the expiratory trigger setting (Active exhalation)
Figure 4 Delayed cycling: Patient inspiratory time is shorter than the expiratory trigger setting (Active exhalation)
4. Double Triggering
This occurs when a single patient's effort delivers two consecutive breaths because of short inspiratory time settings that do not match the patient’s need.13 Or a strong inspiratory effort that activates a second breath immediately.
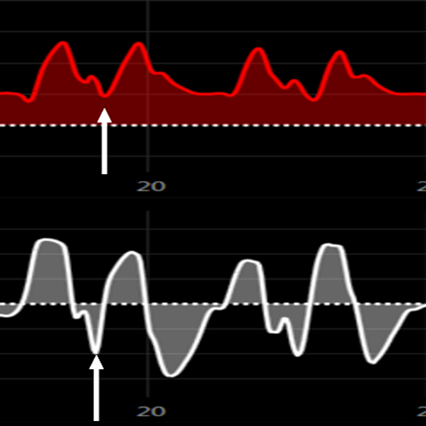 Figure 5 Double Trigger: Breath is terminated early. does not meet the inspiration time of the patient.
Figure 5 Double Trigger: Breath is terminated early. does not meet the inspiration time of the patient.
5. Reverse Triggering
The ventilator initiates a breath, triggering a reflexive diaphragmatic contraction. This can lead to breath stacking, increased tidal volumes, and lung overdistension. 4
Challenges in Mechanical Ventilation
Despite technological advancements, ventilation manufacturers often struggle to translate these issues into effective technical solutions. As a result, ventilators continue to face signal detection challenges in several areas.
Noise and Artifact Interference: Differentiating accurate inspiratory signals from motion artifacts, cardiogenic oscillations, and external noise remains challenging, still leading to false triggering. 7
Air Leak Management: Leaks distort pressure and flow readings, making it difficult for ventilators to identify inspiratory efforts correctly. Those lacking robust leak compensation algorithms may fail to trigger breaths appropriately. 10
Auto-PEEP Detection: Residual pressure (Auto-PEEP) prevents complete exhalation in COPD and obstructive lung diseases. Many ventilators fail to detect Auto-PEEP accurately, often leading to wasted patient efforts. 8
Weak Inspiratory Efforts: Neuromuscular patients or those with severe muscle fatigue generate weak inspiratory signals. Many ventilators struggle to detect these subtle efforts, especially in the presence of noise or leaks. 6
Strategies for Improving Mechanical Ventilators
Manual detection of asynchronies is often impractical or impossible, given that hospitals are often very short on staff. Physicians or respiratory therapists can only review a fraction of the data produced by a ventilator. So, the focus must lie on automated detection systems using machine learning and advanced signal processing algorithms. 14
Despite advancements, developing a universally accepted method for detecting and quantifying asynchrony remains challenging. Variability in waveform interpretation, patient-specific factors, and poor ventilator design pose difficulties and still affect performance, highlighting the need for future strategies to improve synchrony.
Noise and Artifacts
One promising strategy to improve ventilator performance is using signal processing algorithms that differentiate actual patient efforts from background noise, such as cardiogenic oscillations or motion artifacts. Analyzing real-time data and continuously refining pressure modulation based on previous breath cycles, the ventilation controller enhances the ventilator’s ability to synchronize with the patient’s breathing effort. 12
Leak Management
Another essential need for improvement is adequate leak compensation in non-invasive ventilation (NIV). Adjusting the trigger sensitivity dynamically in response to detected leaks to prevent auto-triggering reduces the likelihood of ineffective efforts, which is particularly valuable in detecting efforts accurately in the presence of leaks or external disturbances.
Triggering, Pressurization, and Flow Delivery
Rapidly achieving the target inspiratory pressure is key for ensuring patient-ventilator synchrony. Automating and optimizing rise time aligns ventilator support with the patient’s natural breathing patterns, ultimately improving patient comfort.11 Additionally, low resistance within the ventilator’s gas pathway facilitates pressurization and flow delivery and lowers the work of breathing. Response time, also known as trigger delay, can be optimized by flow waveform analysis to enhance patient comfort and reduce ventilatory inefficiencies.
Auto PEEP
Implementing advanced detection algorithms, expiratory flow control, and machine learning will address the auto-PEEP issue effectively. Further developments in real-time adaptation will enhance the ability to detect and mitigate auto-PEEP, improving synchrony and patient safety. 15
Adaptive Pressure Support
Adaptive pressure support mechanisms refine synchrony by dynamically adjusting ventilatory assistance to match the patient’s inspiratory effort. In ventilatory modes such as NAVA and Proportional Assist Ventilation (PAV), the support is based on real-time patient respiratory system feedback, enabling these modes to provide a more comfortable breathing experience.
Conclusion
Optimizing patient-ventilator interaction requires a multi-faceted approach, including advanced ventilation modes, automated settings, and improved sensing and monitoring. Challenges such as trigger, flow, and cycling asynchronies can be addressed through real-time monitoring, machine learning adjustments, and advanced ventilatory support.
By addressing and executing these requirements, ventilator manufacturers can enhance patient outcomes, improve comfort, and facilitate successful weaning from mechanical ventilation.
References:
Fan, E., Del Sorbo, L., Goligher, E. C., Hodgson, C. L., Munshi, L., Walkey, A. J., ... & Brochard, L. J. (2017). An Official Clinical Practice Guideline from the American Thoracic Society, European Society of Intensive Care Medicine, and Society of Critical Care Medicine: Mechanical Ventilation in Adult Patients with Acute Respiratory Distress Syndrome. American Journal of Respiratory and Critical Care Medicine, 195(9), 1253-1263.
Brochard, L., Slutsky, A., & Pesenti, A. (2017). Mechanical Ventilation to Minimize Progression of Lung Injury in Acute Respiratory Failure. American Journal of Respiratory and Critical Care Medicine, 195(4), 438-442.
3. Georgopoulos, D., Prinianakis, G., & Kondili, E. (2006). Bedside waveform analysis in mechanically ventilated patients. American Journal of Respiratory and Critical Care Medicine, 174(4), 422-433.
4. Akoumianaki, E., Lyazidi, A., Rey, N., Matamis, D., Perez-Martinez, N., Giraud, R., ... & Brochard, L. (2013). Mechanical ventilation-induced reverse triggering in humans. American Journal of Respiratory and Critical Care Medicine, 187(12), 1430-1438.
5. Epstein, S. K. (2005). How often does patient-ventilator asynchrony occur, and what are the consequences? Respiratory Care, 50(2), 183-185.
6. Thille, A. W., Rodriguez, P., Cabello, B., Lellouche, F., & Brochard, L. (2006). Patient-ventilator asynchrony during assisted mechanical ventilation. Intensive Care Medicine, 32(10), 1515-1522.
7. Murias, G., Lucangelo, U., Blanch, L. (2016). Patient-ventilator asynchrony. Current Opinion in Critical Care, 22(1), 53–59. DOI: 10.1097/MCC.0000000000000289
8. Leung, P., Jubran, A., & Tobin, M. J. (1997). Comparison of assisted ventilation modes on indices of patient effort. American Journal of Respiratory and Critical Care Medicine, 155(6), 1940-1948.
9. Richard, J. C., Lyazidi, A., Rey, N., Pili-Floury, S., & Brochard, L. (2012). Measurement of patient-ventilator interaction in the critically ill. Current Opinion in Critical Care, 18(3), 253-258.
10. Burns, K. E., Adhikari, N. K., Meade, M. O., & Slutsky, A. S. (2013). Noninvasive ventilation strategies for acute respiratory failure in adult patients: A systematic review and meta-analysis. Annals of Internal Medicine, 158(3), 173-183.
11. Brouwer, L., Hoedemaekers, A. & van der Hoeven, J. Effect of inspiration rise time on work of breathing and patient comfort during pressure support ventilation. Crit Care 10 (Suppl 1), P38 (2006).
12. T A, G G, P AMD, Assaad M. Machine learning algorithm for ventilator mode selection, pressure and volume control. PLoS One. 2024 Mar 13;19(3):e0299653. doi: 10.1371/journal.pone.0299653. PMID: 38478485; PMCID: PMC10936794.
13. Kallet RH, Campbell AR, Dicker RA, Katz JA, Mackersie RC. Effects of tidal volume on work of breathing during lung-protective ventilation in patients with acute lung injury and acute respiratory distress syndrome. Crit Care Med. 2006;34(1):8‑14.
14. Chatburn RL, Mireles-Cabodevila E. 2019 Year in Review: Patient-Ventilator Synchrony. Respir Care. 2020 Apr;65(4):558-572. doi: 10.4187/respcare.07635. PMID: 32213603.


